At Kieran's Sport Therapy, I want to see people go from strength to strength.
When it comes to sport, injuries are a fact of life. If however you've managed to avoid them up to this point, please tell me your secret! For everyone else, however, managing injuries is something we just have to do. It's pretty simple – my goal, with my sports massage in Southend, alongside rehabilitation prescription, is to help you optimise performance and reduce pain, wherever possible. That's not just for athletes, mind, if you're working a job that has you sitting down all day, back pain can creep up on you before you know it.
No matter what stage of life you're at, no matter how active or inactive, everyone should be able to live pain-free as they go about their day.
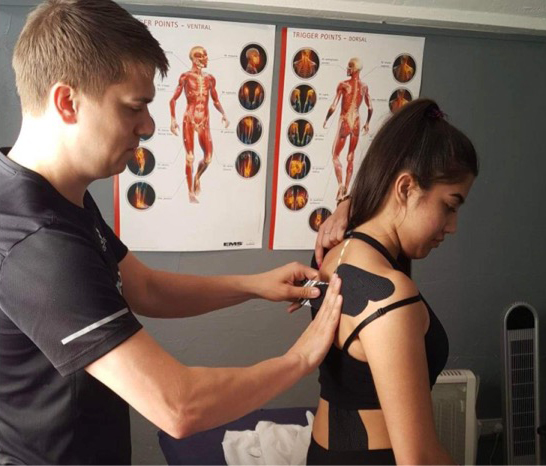
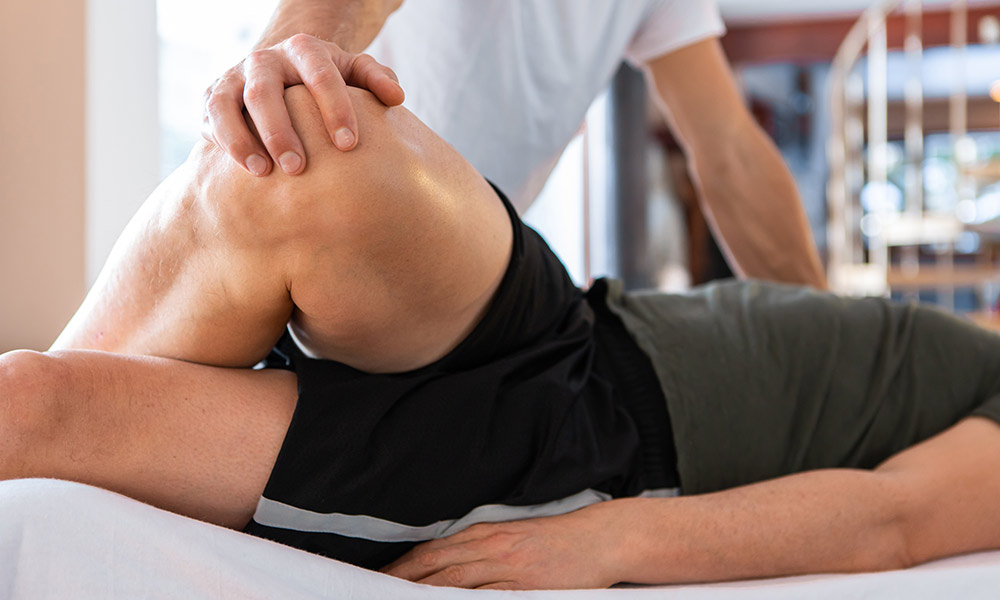
If you're suffering with a niggling injury from any sport or activity you do or if you're feeling the aches and pains that come with a sedentary working life, this is just the thing for you! Take a look at my Sports Therapy and Rehabilitation page to see how I can help get you on the mend!

It's no secret that, in life, the best form of treatment is prevention. The same goes for your body. There's no substitute for a strong, well-conditioned physique when it comes to preventing injury. Check out my Strength and Conditioning page for more info on how this service works!
I always try and keep on top of the sports therapy landscape, to make sure I can provide the best sports massage in Southend.
Take a look at my blog for great tips and tricks on how to train and stay injury-free!
The rehab studio, gym and clinic space I work within are second to none and I provide the best sport massage in Southend. If you're in Leigh on Sea, Westcliff on Sea, Thorpe Bay, Shoeburyness, Great Wakering or any of the surrounding areas, then you're not far away.
Come and see for yourself!
Give me a ring on 07880 883 836 or drop me an email at contact@kieranssporttherapy.co.uk to chat about your injury and arrange a consultation today!